Genital Prolapse
What is genital prolapse?
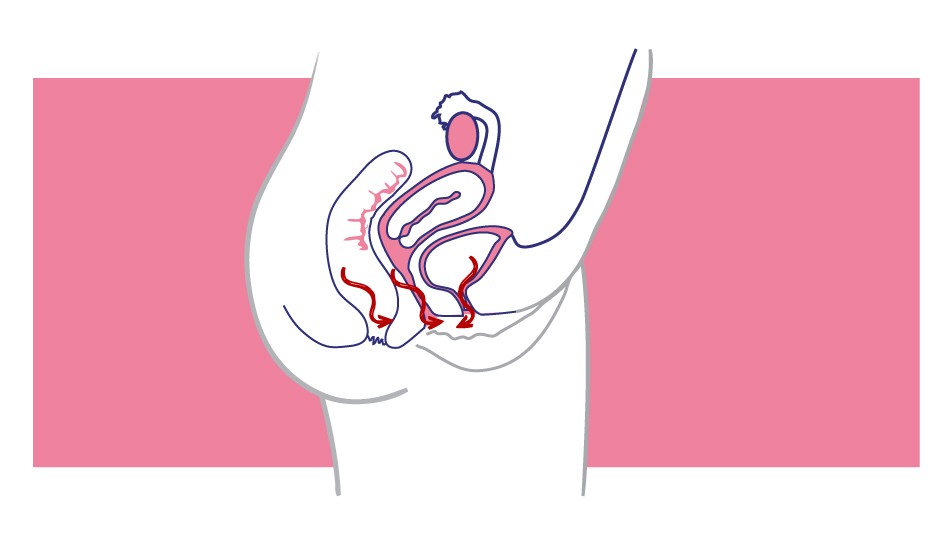
Genital prolapse is the descent of the pelvic organs secondary to the rupture or weakness of the pelvic floor support. It is divided into three types:
Anterior: prolapse of the urethra or bladder, or both, into the vagina (cystocele, uretrocele).
Middle: descent of the uterus or the vaginal vault (uterine prolapse, enterocele).
Posterior: prolapse of the rectum into the vagina (rectocele).
What are the causes of genital prolapse?
Obstetrical trauma, multiparity, babyborn or fetus weight.
“Poor quality” of ligaments, connective tissue and pelvic muscles.
Fall in oestrogen levels, for example in the menopause.
Intra-abdominal pressure aggravated by obesity, respiratory illness, etc.
Previous pelvic surgery.
What are the symptoms of genital prolapse?
Pain in the lower abdomen, sensation of heaviness or pressure in more than 90% of cases.
The sensation of a “lump” in the genital area.
Difficulty, pain or lack of satisfaction in sexual relations.
Pain in the sacro-lumbar region.
Nausea, constipation, defecation disorders.
Difficulty or discomfort when walking or in other physical exercise.
Incontinence or involuntary urine loss, often “taken short”, etc.
How can prolapse be prevented?
It is not known whether it can be prevented. In order to strengthen the pelvic floor and avoid a possible prolapse, it is advisable to practice contraction exercises of the pelvic musculature during pregnancy and the first weeks after giving birth.
What is urinogynecology?
Urinogynecology is a sub-speciality of obstetrics and gynecology for the diagnosis and treatment of pelvic floor disorders. It covers frequent cases such as urinary incontinence and prolapse of the pelvic organs, but is in fact more complicated; it also includes fecal incontinence, bladder evacuation disorders, difficulty in defecation, sexual disfunction and chronic pain. It must therefore be treated conjointly and from a comprehensive and integral point of view.
What is the pelvic floor?
The pelvic floor is all the muscles, ligaments, connective tissue and nerves that support and control the uterus, vagina, bladder, urethra and rectum.
What are the symptoms of pelvic floor disorder?
Urinary incontinence: involuntary loss of urine.
Loss of control of stool and discharge of gases.
Genital prolapse: a condition in which the pelvic organs descend from their normal anatomical position towards the vagina, with the feeling of a “lump” at the level of the external genitalia.
Pelvic pain, soreness or pain in the bladder or urethra.
Disorder or discomfort in sexual relations.
Why is it a social problem?
With the increase of life expectancy, many women are living longer and are therefore more susceptible to pelvic floor disorders, which have unpleasant symptoms that interfere with social relations, travel and sexual activity. They may lead to social isolation, loss of self-esteem and depression.
What is the pelvic floor rehabilitation or physiotherapy?
They are exercises to improve elasticity and muscular strength, to strengthen closure of the urethra and prevent urine loss. The aim is to tone up the muscles of the pelvis, maintain muscular contraction and increase the number of repetitions, and they are known as Kegel exercises. They can be combined with the use of vaginal cones.
What is genital prolapse surgery?
All depicted above is known as advanced reconstructive laparoscopic surgery of the pelvic floor support defects. It requires experience personnel and a skillful surgeon with expertise in laparoscopy. The aim is for patients with problems in the three closely related areas (bladder, uterus, rectum) to be referred to a specialist experienced in the three fields and to treat the problem in a single consultation and a single examination. 20 % of patients require combined procedures that can be dealt with in a single operation.
In this way, both anal incontinence and defecation disorders can be corrected, urinary incontinence treated, anatomy secondary to the prolapse is restored and sexual function is preserved with the aim of improving quality of life.
What are the advantages of surgery by laparoscopy?
A more direct view of the deeper areas of the pelvis is achieved, with easier access to anatomical spaces which are difficult to reach with other types of surgery. This provides better identification and analysis of the support defects, so that sutures are far more precise and effective than with traditional surgery. Blood loss during the operation is much less; post-operative pain is also reduced, with less need for medication; scarring is almost negligible; time spent in hospital is less; recovery is quicker, and the patient can return to work much earlier.