Endometriosis
What is endometriosis?
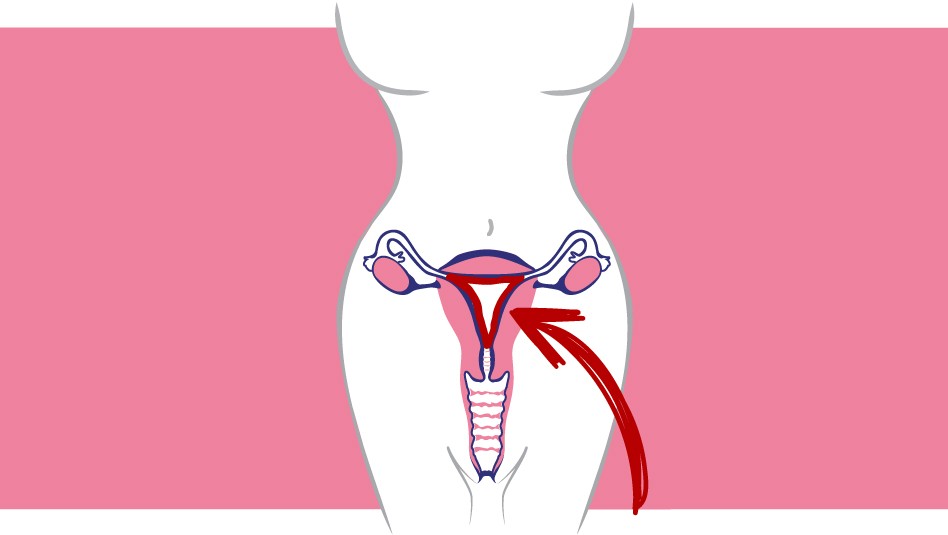
Endometriosis is a benign process characterized by the presence and proliferation of endometrial tissue that is normally found within the uterus, in other different areas outside of this cavity. There are different types:
Ovarian endometriosis: in the ovaries, giving rise to quite large size cysts – endometriomas. These contain a dark brown fluid, which accounts for their name of “chocolate cysts”.
Recto-vaginal septum endometriosis: appears in the recto-vaginal space, the tissue found between the rectum and the vagina. Deep and very active.
Peritoneal endometriosis: affects the peritoneum, the tissue covering the internal organs. It frequently adopts different forms; reddish or brown-coloured patches or small cysts of a dark blue colour. These cysts are often found in the posterior wall of the uterus, but they can also occur in the bladder or intestines.
What are the causes of endometriosis?
The real cause remains unknown. However, the most widely accepted theory is that of retrograde menstruation, the reflux of menstrual fluid to the abdominal cavity and the implantation of endometrial glands in the peritoneum or in the intra-abdominal organs. Most women suffer from it, although it does not result in endometriosis in all cases, thereby pointing to additional factors that lead to the proliferation of endometrial cells. This reflux may begin during puberty, although symptoms may not appear until later. Recent research suggests that certain environmental toxins, such as dioxin, could be responsible for what appears to be a modern epidemic: endometriosis.
As regards genetic predisposition, between 15-20 % of women suffer from this disease. Endometriosis runs in some families. If a mother or daughter have this disease, the chances of another family member developing it is increased seven-fold.
What are the symptoms of endometriosis?
Pain of highly variable intensity during menstruation or coitus; or back pains. Also generalized pelvic pain with abdominal distension. Although this is the most frequent symptom, some women do not suffer from it.
Chronic fatigue
Sterility: between 30-50%
Polycystic ovary disease, uterine miomas, ovarian cysts or congenital or acquired genital malformations.
How is endometriosis diagnosed?
Determined by the presence of pelvic pain, a palpable lump in the pelvis or sterility.Suspects of endometriosis can be confirmed by a surgical laparoscopic procedure. Laparoscopy is the most common surgical procedure for the diagnosis and treatment of endometriosis. This type of operation may also be known as key-hole surgery and is one of the lesser forms of invasive surgical treatment available today.
During this surgical operation under general anaesthetic, a fine endoscope photo-transmitter (laparoscope) is inserted through a tiny incision in the abdomen, just below the navel, it is equipped with lens for a clear view. During a laparoscopic procedure, endometrial implants can be easily seen once these implants have reached a reasonable size. The implants that are still tiny cannot be seen by the naked eye. The surgeon is able to examine the condition of the abdominal organs and verify the size and magnitude of the endometrial tumours, remove endometrial implants, separate any adhesions, also drain and treat or remove large cysts. This method enables other problems presenting similar symptoms to be ruled out.
Other techniques such as ecography, scanning or magnetic resonance may detect the presence of endometriosic lesions in other locations. However, only laparoscopy has so far been able to provide early diagnosis of this disease in women of child-bearing age.
Diagnostic laparoscopy is recommended in the following cases:
Sterile woman under study
Sterility of unknown origin
Abnormalities found during examination of the Fallopian tubes: hysterosalpingography
Patients with pelvic pain
Anomalies in pelvic examination
What is the best form of treatment of endometriosis?
Pharmaceutical treatment
Contraceptives: such as the contraceptive pill or monthly injections, used in the treatment of mild forms of endometriosis and producing few side effects. However, they are not considered effective in more severe cases.
Analogs (aGn-Rh): drugs that reduce the hormonal activity of the ovaries. They are administered over a period of six months, interrupting the production of oestrogen and bringing about a menopause. Endometrial tissue is frequently reduced in size, thereby alleviating pain caused by the disease.
Surgical treatment
Conservative surgical treatment by means of laparoscopy is the most appropriate treatment for patients who wish to bear children, more radical treatment being reserved for hysterectomy and exeresis of both ovaries in patients who do not wish to have children or those with very severe endometriosis.
Advantages
- Less time in hospital
- Less convalescence and faster recovery time
- Lower risk of post-operative adherencies
- Lower risk of infection
- Invisible scars
- Minimally invasive and conservative surgery
- Overall cost reduction
- Use of laser: precise application, depth control, greater destruction of infected cells, minimum blood loss, conservation of reproductive system.
Anaesthetic
General anaesthetic is most commonly employed, given the frequent uncomfortable changes in posture required by this surgical operation, as well as abdominal distension as a result of the gas. Furthermore, thanks to advances in anaesthesia, there is a very low rate of complications.
Risks
Video-laparoscopy ensures a much lower risk of surgical complication than conventional surgery. Multi-centre trials have shown an overall complication rate of 1/1000, the highest incidence being those involving accidents of a digestive nature and haemorrhage. However, these rates are also falling progressively.
Could it be necessary to open the abdomen?
In the course of every endoscopic intervention, the real diagnostic image may differ from that envisaged clinically or by other complementary examinations, thus involving other organs that may make the technical resolution of this operation more difficult. In such cases, it would then be necessary for the benefit of the patient to open the abdomen. This is likely to occur in approximately 5 % of all laparoscopic interventions.